Alternative remedies #3: Is Manuka honey good for eczema?



Honey is well-known as a treatment for sore throats, wounds and infections, due to compounds it contains that kill bacteria. Manuka honey, in particular, is used in licensed wound dressings in the UK. However, value of it in the treatment of childhood eczema is yet to be proved. That said, there’s plenty of anecdotal evidence coming to the fore. Here, we look more closely at Manuka honey and ask whether it’s worth trying it to see if it helps in relieving your child’s eczema.
You may also like to read our review of natural eczema remedies which looks at Manuka honey alongside other traditional eczema remedies.
Manuka honey for eczema
Do a bit of research and you’ll find lots of uses for Manuka honey (besides eating, that is!). From wound care to cancer treatment, the potential benefits of Manuka honey are now being taken seriously by the scientific community. While the value of Manuka honey in the treatment of childhood eczema is yet to be proved, there’s plenty of anecdotal evidence that it can help. We look at the available scientific research into the effectiveness of Manuka honey in treating eczema. And the practicalities of using such a sticky substance on children.

Honey and health
Honey has long been known to have health benefits. The ancient Greeks and Romans were exploiting the healing properties of honey thousands of years ago. It’s known to have an antibacterial quality which helps in wound management. Honey was a popular wound treatment method during the First World War.
More recently, the use of honey in medicine has waned as a result of the introduction of antibiotics. However, it is well-established in the wound dressing industry. It is considered to be helpful in preventing acid reflux, gastroenteritis in infants, treating allergies and infections and relieving colds.
Its wider medical use is relatively unexplored. While honey’s antibacterial qualities are well-known, scientists say that the way it works in fighting infection is not entirely understood. This means the development of honey-based medicine has lagged behind alternative treatments which are understood to a greater degree.
What is known is that the mechanisms of antimicrobial activity of honey are different from antibiotics. Antibiotics typically destroy the bacteria’s cell wall or inhibit intracellular metabolic pathways. The antibacterial activity of honey seems to be due to a number of factors including its acidity and sugar content, which are low enough and high enough respectively to inhibit the growth of most micro-organisms; its hydrogen peroxide component, produced by the glucose oxidase, which again inhibits micro-organism growth; and plant-derived components which can be unique to different kinds of honey (read more here).
It is thought that Manuka honey has antibacterial properties over and above other types of honey. This antibiotic actions may be useful in the treatment of a wide range of illnesses and ailments including, potentially, eczema.
What is Manuka honey and why is it so special?
Manuka honey is produced by bees which gather pollen off the Manuka bush which is native to New Zealand. It can be bought from most supermarkets, health food shops and, of course, Amazon. While certainly delicious, it is rather expensive. You may also come across Kanuka honey, made by bees gathering pollen from Kanuka bushes, a close relation of the Manuka bush.
One of the major antibacterial components in manuka honey is a compound called methylglyoxal (MGO). The flowers of the manuka bush contain a high concentration of a component called dihydroxyacetone (DHA), which is converted into MGO. According to WebMD, ‘the higher the concentration of MGO, the stronger the antibacterial effect.’
Manuka honey is thought to be particularly potent because it has high levels of a compound called dihydroxyacetone, which is present in the nectar of Manuka flowers. This chemical produces methylglyoxal, a compound thought to have antibacterial and cell-killing properties. While research in this area is still in its infancy, the early results are encouraging.
Research in Manuka honey’s benefits
Research has shown Manuka honey to have a ‘broad spectrum of antimicrobial activity and that it is able to act upon more than 80 species of pathogen (a pathogen is a bacterium, virus or other micro-organisms which can cause disease). The NHS says it has been demonstrated that honey can inhibit pathogens normally capable of causing wound infection, including strains that are resistant to conventional antibiotics. In addition, there are early trials suggesting that Manuka honey may be helpful in reducing skin inflammation, which in turn can promote healing. The NHS notes there are a growing number of clinical reports that have shown that wound infections can be cleared by applying Manuka honey directly on the skin, although it points out that medical-grade, purified honey was used in clinical trials on wounds.
Understanding UMF ratings
There are different antibacterial strengths of Manuka honey so in order to guarantee that the honey is of medicinal quality, there is a trademarked rating system called the Unique Manuka Factor (UMF).
Five is the minimum UMF rating you will find but it is worth noting that Manuka honey is generally not considered beneficial below a UMF 10+ rating. UMF 10-15 is useful; however, if you want to treat something, a UMF of 16-20+ is of superior quality and much more effective. Generally, you get what you pay for.
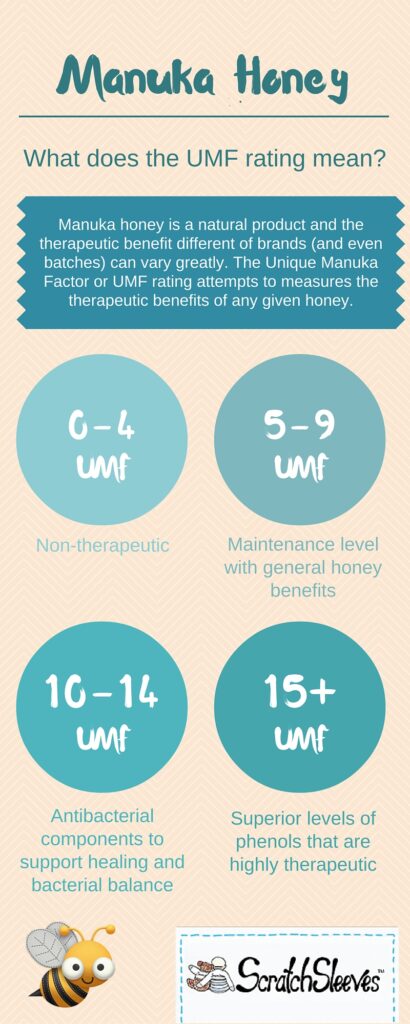
This quick breakdown of UMF ratings can be used to decide the strength you require:
- UMF 0-4 Non-therapeutic
- UMF 5-9 Maintenance level with general honey benefits
- UMF 10-14 Antibacterial components to support healing and bacterial balance
- UMF 15+ Superior levels of phenols that are highly therapeutic. Do not exceed 1 tablespoon at a time at this level.
Other rating systems are in use so do check which system is being used when purchasing – you can find more information here.
Using Manuka honey to treat eczema
Officially, the jury is still out because there is no conclusive scientific evidence that manuka honey can cure or alleviate eczema in children.
However, a small study carried out in 2017 did conclude that manuka honey has potential as an effective eczema treatment. The study involved adult volunteers with eczema applying manuka honey to an affected area of the skin every night for seven days. They left another patch of affected skin untreated to act as the control. The results of the study were that ‘the atopic dermatitis lesions significantly improved post manuka honey treatment versus pre-treatment as compared to control lesions.’ Because the study was small, it concluded that the results need to be confirmed by randomized and controlled clinical trials.
Application of Manuka honey to the skin is thought to help eczema by:
- Keep the skin moist which helps to reduce or remove the incidence of eczema flare-ups
- Acting as a humectant, drawing moisture from deep within the skin to the dry surface layers
- Reducing inflammation, which in turn can aid healing
- Inhibiting the growth of harmful bacteria, including Staphylococcus, commonly found on eczema-prone skin
- The high viscosity of honey is also thought to form a barrier for the skin which is helpful in preventing infection in the first place.
Consumption of Manuka honey is also thought to boost the immune system. It makes sense to foster a healthy immune system when trying to reduce the impact of eczema.
Applying Manuka honey to the skin – is it practical?
Honey is certainly a sticky substance so if you want to apply it directly to the skin, do so sparingly!
Here’s how to make your own honey dressing:
- Wash your hands.
- Put a layer of medical-grade honey on your itchy spots.
- Cover with a sterile gauze or bandage.
- Leave on overnight.
- Wash off with warm water and pat dry
Do this every night for 1 week.
If keeping the honey in place over night is impractical, aim for at least 20 minutes. Distract them with a story or their favourite TV show while the honey works its magic. For treating hands or arms, you could apply the honey at bedtime, cover with a set of ScratchSleeves and then rinse it off in the morning.
If you wet wrap your child’s eczema-affected skin you could try using the Manuka honey as the moisturising layer.
- Top tip: Warming the honey slightly before you apply it will make it easier to spread and less likely to drag on the skin as you apply it.
Manuka honey in other products
If you just can’t face the stickiness, there are a number of creams available which include Manuka honey. However, as with all un-regulated skincare products, do check the packaging. Make sure that the honey appears at or near the top of the ingredients list to be sure that the cream contains enough to be beneficial.
Alternatively, you can make your own cream using 1 part beeswax to 10 parts coconut oil and 10 parts honey. Melt the beeswax, add the coconut oil and melt that too. Stir in the honey and whisk until the cream is smooth. Decant into a sterilised jar and allow to cool.
Feeding your child Manuka honey is less likely to be a problem! You could try spreading on toast or bread, adding to their yoghurt or topping their cereal.
Are there any disadvantages?
Fortunately, honey is relatively free of adverse effects so most parents of children with eczema will be able to try it out to see if it helps.
It is however worth noting that the NHS does not recommend giving honey to children under the age of one . This is because honey can occasionally contain a bacteria that can cause infant botulism.
Applying honey to the skin can occasionally result in a slight stinging sensation, but this wears off very quickly.
Allergy to honey is rare it is possible to be allergic to either pollen or bee proteins in honey.
Plus, don’t over-use as excessive application of honey may lead to dehydration of tissues.
Our conclusion
While there’s little scientific evidence that Manuka honey is an effective treatment for eczema in children, our conclusion is that Manuka honey is certainly worth a try. If it doesn’t work at least you can enjoy eating it – it’s delicious!
Our sources
- Traditional and Modern Uses of Natural Honey in Human Diseases: A Review. T Eteraf-Oskouei1, M Najafi. Iranian Journal of Basic Medical Science. 2013 Jun; 16(6): 731–742.
- Topical application of natural honey, beeswax and olive oil mixture for atopic dermatitis or psoriasis: partially controlled, single-blinded study.
Al-Waili NS, Complementary Therapies in Medicine 2003; 11(4): 226–234 - Potential pathway of anti-inflammatory effect by New Zealand honey. Tomblin V, Ferguson LR, Han DY, Murray P, Schlothauer R. International Journal of General Medicine. 2014 Mar 5;7:149-58
- A randomised controlled trial of topical Kanuka honey for the treatment of eczema. J Fingleton, C Helm, C Tofield, M Weatherall, R Beasley. Journal of the Royal Society of Medicine. 2014 Jan; 5(1)
Our Editorial Policy
Here at ScratchSleeves, we aim to bring you trustworthy and accurate information. We collaborate with qualified dermatologists and doctors as well as drawing on peer-reviewed medical studies and our own experience as parents. All medical content is reviewed by a dermatologist or appropriate doctor prior to publication to ensure completeness, accuracy and appropriate use of medical language. Reviewer details can be found at the bottom of each reviewed post and also on our ‘Meet The Team’ page.
All scientific research referred to in our blog is found in peer-reviewed publications. All the eczema related medical articles we refer to are included in the GREAT database (Global Resource of Eczema Trials) managed by the ‘Centre of Evidence Based Dermatology’ at the University of Nottingham. This database brings together information on all randomised control trials and systematic reviews of eczema treatments. Trials are identified using a highly sensitive, comprehensive search strategy that is compatible with standard Cochrane methodology. Cochrane is internationally recognised as the highest standard in evidence-based health care. Links to the publications we refer to are listed at the bottom of each article.
Disclaimer
The original editorial information we provide is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your doctor or other qualified healthcare practitioners regarding a medical condition. Never disregard professional medical advice or delay in seeking it in because of anything you have read on the ScratchSleeves blog.
As well as sharing our experience of bringing up an eczema child (and favourite allergy-friendly recipes), ScratchSleeves also manufacture and sell our unique stay-on scratch mitts and PJs for itchy babies, toddlers and children. We now stock sizes from 0-adult in a range of colours. Visit our main website for more information.
The Calm Skin Guide
Love our blog? It's also available in book format with:
- First hand accounts from parents & medical professionals
- Easy navigation
- Comprehensive index
- Additional material
Signed copies available at no extra cost
Written by:
Reviewed by:
Interesting article? Don't keep it to yourself...
Read next...
You may also find helpful...
Quick buy


Multi Buy Discount

Spend between £30 - £60 and save 5%
Spend between £60 - £120 and save 10%
Spend over £120 and save 15%
Discount automatically applied at checkout
No Quibbles Guarantee

ScratchSleeves abide by a no quibbles guarantee.
Free UK Postage

Free packing and postage on all UK orders. For overseas orders to Europe postage is from £3.50, to USA is £6.50 and to the rest of the world, from £3.75.







